Introduction
Early recovery after a kidney transplant is often described through lab numbers, medication schedules, and clinic visits. Those medical markers are important, but they rarely capture how recovery actually feels for the patient living through it.
If you have already gone through the early phase described in Kidney Transplant Recovery: The First Weeks After Surgery, you may realize that much of recovery is not dramatic—it is gradual, quiet, and deeply personal.
For me, one such quiet but meaningful milestone came during a routine follow-up appointment. It was the day my surgical drain tube and ureteric stent were finally removed.
As a kidney transplant recipient myself, I remember how these small devices shaped the first weeks of my recovery in ways I had not expected.
From a surgical perspective, these devices are temporary supports. But for a transplant recipient, their removal often signals that the most fragile phase of recovery is beginning to settle.
Looking back, that day represented more than a minor procedure. It marked a transition—when the transplanted kidney started to feel less like a surgical graft and more like part of my normal life again.
Understanding the Purpose of the Drain Tube and Ureteric Stent
After kidney transplant surgery, surgeons often place temporary devices to protect the new kidney and support healing during the early postoperative period.
These devices are not signs of complications. Instead, they are preventive measures designed to reduce surgical risks while the body adapts to the transplanted organ.
Two of the most common supports used during this stage are the surgical drain tube and the ureteric stent.
1. The Surgical Drain Tube
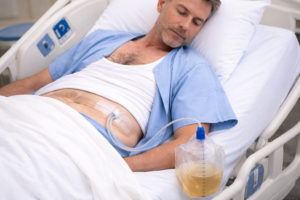
A surgical drain is placed near the transplant site to remove fluid that naturally accumulates after surgery.
This fluid may include small amounts of blood, lymphatic fluid, and inflammatory exudate produced as tissues heal. Without drainage, these fluids could collect around the transplanted kidney, create pressure, and increase the risk of infection.
The drain allows doctors to monitor fluid output and helps prevent these collections from interfering with the early healing process.
In most transplant centers, the drain remains in place for several days until fluid production decreases to a safe level. However, as I learned personally, timelines do not always follow the average.
2. The Ureteric Stent
The ureter is the tube that carries urine from the kidney to the bladder. During transplant surgery, the donor kidney’s ureter must be surgically connected to the recipient’s bladder.
A temporary ureteric stent is placed inside this connection to keep it open while healing occurs.
The stent acts like an internal support structure. It helps prevent obstruction, leakage, or narrowing at the surgical junction.
Unlike the drain tube, the stent remains inside the body and is usually removed a few weeks after surgery once the connection has stabilized.
Living With the Drain and Stent During Early Recovery
In the first weeks after transplant, these devices quietly shape many small aspects of daily life.
For me, the drain tube was actually a surprise. When I woke up from general anesthesia, I noticed a tube coming out from the side of my abdomen connected to a small collection bag.
No one had mentioned it to me clearly beforehand—not during discussions with other patients or during counseling. That moment stayed with me because it showed how even well-prepared patients can still encounter unexpected realities.
The drain tube becomes a constant physical reminder that your body is still healing. Movements become slower and more deliberate. Even turning in bed requires awareness.
There is also a behavioral shift. You start paying attention to drain output, numbers, and patterns—things that never mattered before.
In many patients, the drain is removed before discharge. But in my case, the fluid output remained higher than expected, so I went home with the drain still in place. That changed daily life more than I anticipated.
I had to carry the drainage bag everywhere. Simple actions required planning. My transplanted kidney was on the right side, and the drain exited from the same area, causing irritation and mild inflammation over time.
Sleeping was particularly difficult. For nearly two weeks, I could not comfortably lie on either side.
Eventually, about ten days after discharge, the fluid decreased and the drain was removed.
The ureteric stent was different. I rarely felt it during daily activities. Occasionally, there was mild awareness during urination, but overall it remained subtle—almost invisible in daily life.
The Day of Removal
The removal of the drain tube and ureteric stent usually happens in separate stages.
Medically, both are simple procedures. But emotionally, they carry more weight than expected.
1. Drain Removal
Drain removal is usually done in the clinic once fluid output drops to a safe level.
The procedure is brief. The tube is gently pulled out, creating a short pulling sensation that lasts only a few seconds. Physically, it is minor. But psychologically, it is noticeable.
After living with the drain, its removal felt like removing a visible symbol of surgery. Movement became easier. There was less constant awareness of the surgical site.
In my case, that moment felt quietly relieving—more than I had anticipated.
2. The Ureteric Stent Removal
Stent removal is typically done through a short cystoscopy. A flexible camera is passed through the urethra into the bladder. The stent is then grasped and removed.
Before the procedure, a local anesthetic gel is applied. Because of that, I did not feel pain during insertion.
The procedure itself was quick. What stayed with me was not discomfort, but the anticipation beforehand.
Afterward, I noticed a temporary change in urinary sensation. For a brief moment, urine flow felt delayed. I was advised to increase hydration, and normal function returned quickly.
My stent was removed on day 21 post-transplant.
What This Milestone Meant to Me
The day itself was not dramatic. There was no celebration. No clear “turning point” moment.
It was just another hospital visit. But internally, something shifted.
The drain had been a constant reminder of vulnerability. Its removal reduced that awareness. The stent removal added another layer of reassurance. These were small changes, but together, they signaled progress.
If you look at recovery in a broader sense, like in Kidney Transplant Recovery Timeline: What Really Happens Week by Week, this stage sits between early fragility and gradual stabilization.
You don’t feel fully recovered—but you no longer feel immediately post-surgical either.
Psychological Meaning of This Milestone
Early transplant recovery often carries a quiet anxiety. You monitor medications, hydration, urine output, and lab values constantly. The kidney feels precious, but also fragile.
Milestones like this help rebalance that mindset. The removal of temporary supports sends a message—not verbally, but physically—that healing is progressing.
It helps shift your thinking from:
“I am recovering from surgery to I am learning to live with this kidney”
That transition is subtle, but important.
If you’ve noticed emotional fluctuations during this phase, it’s not unusual. It connects closely with what I discussed in Mental Health After Kidney Transplant: The Hidden Recovery.
Practical Guidance After Stent Removal
1. Maintain Hydration
After stent removal, hydration becomes even more important. It helps flush the urinary system and supports stable kidney function.
2. Monitor Urinary Changes
Mild burning or a small amount of blood in urine can occur briefly. These usually settle quickly. Persistent symptoms should not be ignored.
3. Stay Consistent With Medications
Nothing changes in your immunosuppressive regimen. If anything, consistency becomes more important as visible supports are removed. This connects directly with Kidney Transplant Medications: My Daily Reality and What to Expect.
When to Seek Medical Advice
Even though these procedures are routine, certain symptoms should prompt early contact with your transplant team:
- Persistent fever
- Increasing abdominal pain
- Heavy or prolonged blood in urine
- Difficulty urinating
- Redness or discharge at the surgical site
In transplant care, early communication is always safer than waiting.
Frequently Asked Questions
Is ureteric stent removal painful after kidney transplant?
Most patients describe it as uncomfortable rather than painful. The idea of the procedure often causes more anxiety than the procedure itself. With local anesthesia, the actual process is brief and manageable.
How long does the stent stay after kidney transplant?
In most transplant programs, it remains for about three to six weeks. The exact timing depends on surgical technique, healing progress, and institutional protocol.
Is drain tube removal painful?
It usually causes a short pulling sensation that lasts only a few seconds. The anticipation is often worse than the actual experience.
Can I return to normal activities after stent removal?
Most daily activities can resume fairly quickly. However, recovery is still ongoing, and it’s important not to overestimate your readiness. Gradual progression remains key.
Conclusion
Kidney transplant recovery does not move in big, dramatic steps. It moves through small, often unnoticed transitions. Over time, these small milestones build confidence.
The removal of the drain tube and ureteric stent is one of those transitions. Medically, it reflects stable healing. Psychologically, it reduces the constant reminder of surgery. And that confidence becomes the foundation for long-term stability.
Recovery is not about reaching a single moment where everything feels “normal” again. It is about gradually learning to trust your body, your routine, and your new kidney—step by step.
About the Author
Dr. Salman is a veterinarian (DVM, M.Phil.) and kidney transplant recipient since August 2023.
Through RenalRenewal.com, he shares his personal transplant journey along with medically responsible explanations to help patients better understand recovery, medications, and life after transplant.
Medical Disclaimer
The content on RenalRenewal.com reflects my personal experience as a kidney transplant recipient along with general educational information.
I am a veterinarian (DVM, M.Phil.), not a licensed medical doctor for human healthcare.
This website does not provide medical diagnosis or treatment. Always consult your transplant team or qualified healthcare provider for medical advice specific to your condition.
